Rocky Mountain Spotted Fever – Diagnosis and Treatment
Environmental Injuries / Exposures, Infections
First 5 Minutes
- Rocky Mountain spotted fever (RMSF) can be severe and fatal (case fatality 5-10%) if not recognized and treated early with doxycycline (1).
- There should be clinical suspicion of RMSF in patients with nonspecific febrile illness and sepsis of unclear etiology, especially during spring and summer (1).
Context
- Rocky Mountain spotted fever (RMSF) is rickettsial disease caused by the bacteria Rickettsia rickettsii which get transmitted through tick bites (1).
- RMSF is common in the United States, Western Canada, Mexico, Panama, Costa Rica, Argentina, Brazil, Colombia and Bolivia and it is the most common tick-borne disease in the United States (6).
- Symptoms of RMSF typically appear 3–12 days after the bite of an infected tick or between the 4th and 8th day after discovery of an attached tick (1,2).
- The most common initial signs and symptoms include fever, headache, chills, malaise, myalgia, nausea, vomiting, abdominal pain, photophobia, anorexia (1,2).
- Infection with R. rickettsii leads to systemic vasculitis that manifests as petechial skin lesions which typically appear 2-4 days after fever onset, shown in figure 1 (1).
- Late-stage manifestations include noncardiogenic pulmonary edema (acute respiratory distress syndrome [ARDS]), cerebral edema, acute renal failure, hyponatremia, shock, and seizure (1,4,5).
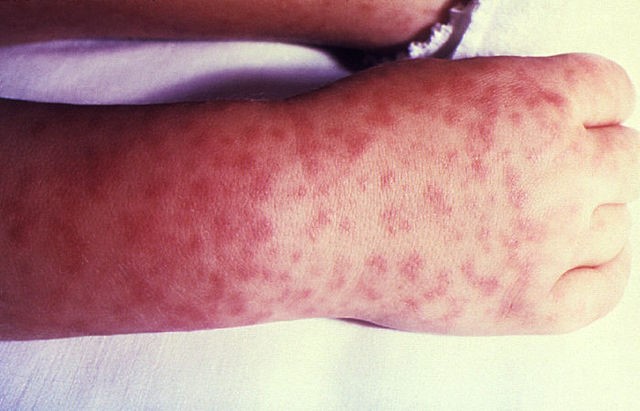
Figure 1. Maculopapular rash with central petechiae in a patient with RMSF. Image accessed from Wikimedia Commons. (https://commons.wikimedia.org/wiki/File:Rocky_Mountain_spotted_fever_PHIL_1962_lores.jpg)
Laboratory Findings
- Total white blood cell count is typically normal or slightly increased in patients with RMSF and increased immature neutrophils are often observed (1,3).
- Thrombocytopenia, elevations in hepatic transaminases (aspartate transaminase and alanine transaminase), and hyponatremia might be present, particularly as the disease worsens (3).
- Elevated creatinine kinase or lactate dehydrogenase may be present later in the course of the disease and indicates diffuse tissue injury (1,3).
- Laboratory values alone cannot be relied on to guide early treatment decisions because they are often close to normal early in the course of illness (3).
Diagnostic Process
- Diagnosis of RMSF is made based on history, physical examination, and laboratory results (1,3).
- A detailed history should be taken to elicit information such (1):
- Travel history within and outside Canada.
- Travel to an area where tickborne rickettsial disease are endemic within 2 weeks of symptom onset supports presumptive diagnosis.
- Known tick bites or activities with exposure to ticks (gardening, walking dogs, hiking, visiting parks).
- Contact with pets, especially dogs, with history of tick attachment or recent tick removal.
- Diagnostic tests for rickettsial diseases, particularly RMSF are not helpful in making a timely diagnosis and should not delay initiating treatment (1).
Recommended Treatment
- Doxycycline is the first-line treatment for RMSF and all other tickborne rickettsial diseases, including children aged <8 years (1).
- Recommended dosing of doxycycline (orally or intravenous) (1):
- Adults: 100mg BID
- Children < 45kg: 2.2mg/kg BID
- The recommended duration of therapy is a minimum of 5-7 days, or at least 3 days after fever resolves and when there is evidence of overall clinical improvement (1).
- Oral therapy is appropriate in early stages of disease who can be treated as outpatients and intravenous therapy is indicated for more severe cases who require hospitalization, particularly those who are vomiting or obtunded (1).
- It is crucial to arrange close follow-up with patients treated as outpatients to ensure they are responding to therapy.
- Studies don’t support prophylactic antibiotics in patients with recent tick bite who are not ill (7).
- The only other antibiotic to treat RMSF is Chloramphenicol, but there is a higher risk of death in patients treated with Chloramphenicol compared to tetracyclines.
Criteria For Hospital Admission
- Hospitalization should be considered for patients with evidence of organ dysfunction, severe thrombocytopenia, mental status changes, or need for supportive therapy (1).
- Other factors to consider when admitting patients include likelihood that the patient can and will take oral medications and the patient’s immune status (1).
- Severely ill patients should be admitted to the internal medicine service for ongoing assessment of fluid status and electrolytes, especially when with hypotension or renal failure (1).
Criteria For Transfer To Another Facility
- Dependent on local guidelines. In general, transfer may be considered if:
- Patient care requirements exceed hospital capabilities (e.g., cardiac monitoring, intensive care, pediatric or maternal care, etc.).
- Treatment is not available and cannot be delivered to current facility.
- Specialist consultations are required and not available at current facility.
Criteria For Close Observation And/or Consult
- Consult the infectious disease consult service.
Criteria For Safe Discharge Home
- If patients are discharged for outpatient treatment, they must have close follow-up to ensure they are responding appropriately to therapy.
Quality Of Evidence?

High
We are highly confident that the true effect lies close to that of the estimate of the effect. There is a wide range of studies included in the analyses with no major limitations, there is little variation between studies, and the summary estimate has a narrow confidence interval.
Moderate
We consider that the true effect is likely to be close to the estimate of the effect, but there is a possibility that it is substantially different. There are only a few studies and some have limitations but not major flaws, there are some variations between studies, or the confidence interval of the summary estimate is wide.
Low
When the true effect may be substantially different from the estimate of the effect. The studies have major flaws, there is important variations between studies, of the confidence interval of the summary estimate is very wide.
Justification
- There is no data from randomized controlled trials that support the use of doxycycline for RMSF. Much of the published literature is more than 20 years old. Only peer-reviewed publications and published guidelines were used for this summary.
Related Information
OTHER RELEVANT INFORMATION
- For More In-depth Review
- BCCDC webpage on Rickettsial Disease: http://www.bccdc.ca/health-info/diseases-conditions/rickettsial-diseases
- For More In-depth Review
Reference List
Biggs HM, Behravesh CB, Bradley KK, et al. Diagnosis and Management of Tickborne Rickettsial Diseases: Rocky Mountain Spotted Fever and Other Spotted Fever Group Rickettsioses, Ehrlichioses, and Anaplasmosis — United States. MMWR Recomm Rep 2016;65(No. RR-2):1–44. DOI: http://dx.doi.org/10.15585/mmwr.rr6502a1
Wolbach SB. Studies on Rocky Mountain spotted fever. J Med Res. 1919;41:1–198.41.
Traeger MS, Regan JJ, Humpherys D, et al. Rocky Mountain spotted fever characterization and comparison to similar illnesses in a highly endemic area—Arizona, 2002–2011. Clin Infect Dis 2015;60:1650–8. http://dx.doi.org/10.1093/cid/civ115
Valbuena G, Walker DH. Infection of the endothelium by members of the order Rickettsiales. Thromb Haemost 2009;102:1071–9.
Kaplowitz LG, Robertson GL. Hyponatremia in Rocky Mountain spotted fever: role of antidiuretic hormone. Ann Intern Med 1983;98:334–5. http://dx.doi.org/10.7326/0003-4819-98-3-334
Chen LF & Sexton DJ. What’s new in Rocky Mountain spotted fever? Infectious Disease Clinics of North America 2008;22(3):415-32, vii-viii. doi:10.1016/j.idc.2008.03.008
Clements ML, Dumler JS, Fiset P, et al. Serodiagnosis of Rocky Mountain spotted fever: comparison of IgM and IgG enzyme-linked immunosorbent assays and indirect fluorescent antibody test. J Infect Dis 1983;148:876–80. http://dx.doi.org/10.1093/infdis/148.5.876
RESOURCE AUTHOR(S)

DISCLAIMER
The purpose of this document is to provide health care professionals with key facts and recommendations for the diagnosis and treatment of patients in the emergency department. This summary was produced by Emergency Care BC (formerly the BC Emergency Medicine Network) and uses the best available knowledge at the time of publication. However, healthcare professionals should continue to use their own judgment and take into consideration context, resources and other relevant factors. Emergency Care BC is not liable for any damages, claims, liabilities, costs or obligations arising from the use of this document including loss or damages arising from any claims made by a third party. Emergency Care BC also assumes no responsibility or liability for changes made to this document without its consent.
Last Updated Dec 29, 2022
Visit our website at https://emergencycarebc.ca
COMMENTS (0)
Add public comment…


POST COMMENT
We welcome your contribution! If you are a member, log in here. If not, you can still submit a comment but we just need some information.