Monkeypox for the Emergency Clinician
Infections
Context
Background:
- Monkeypox is an endemic disease in the Congo Basin and West Africa.
- In May of 2022, there were reports of community transmission of monkeypox in London, England which eventually spread to North America.
- 2 distinct types/clades: Congo Basin clade of the virus has a case fatality of 1 – 10%, the West Africa clade has a case fatality rate of 1%.
- Names of these clades will likely be renamed by the World Health Organization (WHO) to avoid stigmatization.
- Monkeypox is member of the poxviridae family which includes molluscum contagiousum, vaccinia and smallpox.
- First case was identified in 1970 in a 9-year old boy in the Democratic Republic of Congo.
- Despite the name and the fact it was initially identified in monkeys, the exact animal reservoir is unknown.
- As of June 14, 2022 there have been 1600 confirmed cases, 1500 suspected cases and 72 deaths in 39 countries.
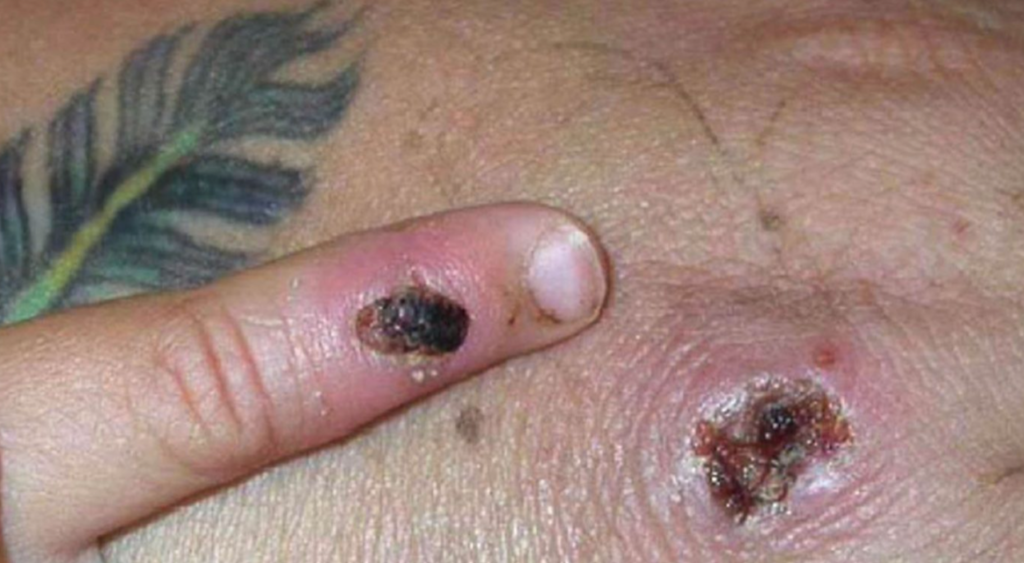
Monkeypox lesion. Photo: CDC
Transmission:
- Limited data available.
- Likely spread from infected animals to humans either directly or indirectly through bites, scratches, hunting, skinning.
- Human to human transmission through direct contact with infectious skin or lesions, respiratory droplets and possibly short range aerosols.
- Potential fomite transmission through contaminated clothing, linen.
- High proportion of cases identified in patients who identify as gay, bisexual and men who have sex with men – potentially related to positive health behaviours and strong connections to STI resources.
Clinical Presentation:
- Non-specific viral illness, less dramatic and often fewer lesions than smallpox.
- First phase (1 -5 days): fever, headache, myalgias, lymphadenopathy.
- Second phase (1-3 days): fever subsides and rash appears which progresses in a stereotypical fashion – macule, papule, vesicle, pustule, umbilicate lesion, crusting and desquamation.
- Rash typically starts on the face and extended to the palms, soles and feet, mucous membranes.
- 75% of cases in North America and Europe present initially with genital lesions.
- Risk factors for severe disease: viral DNA count, number of skin lesions, AST and ALT on day of diagnosis.
Differential Diagnosis:
- Viruses: HSV, VSV, molluscum contagiousum.
- Bacteria: MRSA.
- STIs: syphilis, lymphogranuloma venereum, granuloma inguinale.
Recommended Treatment
Management:
- Place patient in negative pressure room with airborne, droplet and contact precautions for all patient encounters.
- Call infection prevention and control, medical microbiology and infectious disease consulting services.
- Report case to regional public health office.
- Exposed contacts (including healthcare workers without adequate PPE) should self-monitor for 21 days.
- Lesions should be de-roofed and at least 2 lesions and an oropharyngeal swab should be taken using standard red collection tubes.
- Mainstay of treatment is supportive care and analgesia.
- Tecovirimat is an anti-viral licensed for the treatment of smallpox – may be used for more severe cases as per infectious diseases under special use authorization.
- As per the World Health organization, potential post-exposure prophylaxis with IMVAMUNE, a live attenuated, non-replicating smallpox vaccine up to 2 weeks after an exposure to a potential or confirmed case.
Treatment not recommended:
- Prophylactic antibiotics unless overlying skin and soft tissue infection.
Quality Of Evidence?

High
We are highly confident that the true effect lies close to that of the estimate of the effect. There is a wide range of studies included in the analyses with no major limitations, there is little variation between studies, and the summary estimate has a narrow confidence interval.
Moderate
We consider that the true effect is likely to be close to the estimate of the effect, but there is a possibility that it is substantially different. There are only a few studies and some have limitations but not major flaws, there are some variations between studies, or the confidence interval of the summary estimate is wide.
Low
When the true effect may be substantially different from the estimate of the effect. The studies have major flaws, there is important variations between studies, of the confidence interval of the summary estimate is very wide.
Justification
Low – this is an ongoing outbreak with little clinical data to support the current recommendations.
Related Information
OTHER RELEVANT INFORMATION
Nalca A, Rimoin AW, Bavari S, Whitehouse CA. Reemergence of monkeypox: prevalence, diagnostics, and countermeasures. Clin Infect Dis 2005; 41:1765.
World Health Organization. Monkeypox fact sheet. https://www.who.int/news-room/fact-sheets/detail/monkeypox (Accessed on May 23, 2022).
United States Centers for Disease Control and Prevention. https://www.cdc.gov/poxvirus/monkeypox/response/2022/world-map.html (Accessed on June 10, 2022).
Mauldin MR, McCollum AM, Nakazawa YJ, et al. Exportation of Monkeypox Virus From the African Continent. J Infect Dis 2022; 225:1367.
United States Centers for Disease Prevention and Control. Monkeypox: monitoring people who have been exposed. https://www.cdc.gov/poxvirus/monkeypox/clinicians/monitoring.html#exposure (Accessed on May 24, 2022).
RESOURCE AUTHOR(S)

DISCLAIMER
The purpose of this document is to provide health care professionals with key facts and recommendations for the diagnosis and treatment of patients in the emergency department. This summary was produced by Emergency Care BC (formerly the BC Emergency Medicine Network) and uses the best available knowledge at the time of publication. However, healthcare professionals should continue to use their own judgment and take into consideration context, resources and other relevant factors. Emergency Care BC is not liable for any damages, claims, liabilities, costs or obligations arising from the use of this document including loss or damages arising from any claims made by a third party. Emergency Care BC also assumes no responsibility or liability for changes made to this document without its consent.
Last Updated Jun 15, 2022
Visit our website at https://emergencycarebc.ca
COMMENTS (0)
Add public comment…


POST COMMENT
We welcome your contribution! If you are a member, log in here. If not, you can still submit a comment but we just need some information.