Aphthous Ulcer
Ears, Eyes, Nose, and Throat, Gastrointestinal, Hematological / Oncological, Infections, Inflammatory, Metabolic / Endocrine
Context
Aphthous ulcer (aphtha = “mouth ulcer”) tends to be a misnomer.
That is, it is still in common use and is more accurately described in the literature as Recurrent Aphthous Stomatitis (RAS), due to its recurrent nature. It is also known as Recurrent Aphthous Ulcers or Canker Sores.
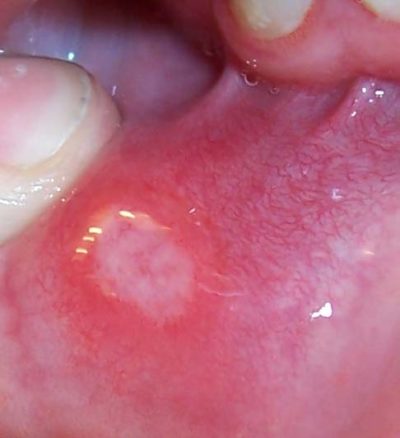
- Recurrent Aphthous Stomatitis (RAS) are ulcers of the oral mucosa that are painful, round, and have an erythematous “halo”.
- About 20% of the population is affected, with the peak age of onset between 10 – 19 years.
- Frequency declines with aging and may spontaneously disappear beyond 30 years.
RAS may present as Minor, Major, or Herpetiform ulceration, with most patients presenting in the latter two categories.
Minor Aphthous Ulcers:
-
-
- 80% of RAS.
- Less than 1 cm.
- Occur on nonkeratinized oral mucosae (Buccal/lip mucosae, floor of mouth, ventral surface of tongue).
- Yellow-grayish pseudomembranous center.
- Burning prodrome 1-2 days prior.
- Heal spontaneously with no scarring in 10-14 days.
-
Major Aphthous Ulcers:
-
-
- Larger than 1 cm.
- May occur on keratinized oral mucosae (Dorsum of tongue, hard palate).
- May last weeks to months and heal with scarring.
- Herpetiform Aphthous Ulcers:
- Clusters of multiple pinpoint ulcers.
- Occur scattered throughout the mouth.
- Typically lasts less than 30 days and is unlikely to scar.
-
- Precipitating factors:
- Trauma to site.
- Smoking cessation.
- Anxiety or Stress.
- Menstrual cycle hormonal changes.
Diagnostic Process
- Diagnosis is based on:
- History of recurrent ulcers.
- Characteristic lesions (dependent on type of aphthous stomatitis).
- Generally painful, yellow-grayish pseudomembranous center with erythematous halo.
- Ulcers lasting 3 weeks or longer require further work-up to rule out other serious causes.
- Lab investigations are not required UNLESS history and physical exam are highly suggestive of an alternate/secondary diagnosis such as:
- Infectious:
- Frequent recurrence, slower healing, and larger lesions suggest immunocompromised state.
- Rheumatic:
- Genital or other extraoral lesions.
- Joint involvement.
- Dermatological:
- Cutaneous lesions.
- Uncharacteristic shape of lesion.
- Hematologic:
- Recurrent fever.
- Inflammation in other areas of the body.
- Bone pain.
- Anemia.
- Petechiae or purpura.
- Gastrointestinal:
- Persistent diarrhea.
- Weight loss.
- Abdominal pain.
- Infectious:
- Differential Diagnosis:
- Infectious:
- HIV.
- Herpesvirus.
- Rheumatic:
- Behçet’s syndrome.
- Reiter’s syndrome.
- Sweet’s syndrome.
- Dermatological:
- Erythema multiforme.
- Pemphigus or pemphigoid.
- Hematologic:
- Cyclic neutropenia.
- Leukemias.
- Gastrointestinal:
- Celiac disease.
- Inflammatory bowel disease (Ulcerative colitis, Crohn’s disease).
- Infectious:
-
Possible investigations guided by secondary findings:
- CBC.
- HIV/Other virologic testing.
- Nutritional deficiencies (Vitamin B12, folate, iron).
- Antigliadin/Transglutaminase antibodies.
-
C Reactive Protein/ESR.
Recommended Treatment
- The goal of therapy is to reduce pain and inflammation.
- Choice of therapy is based on the severity of pain, frequency, size, and number of ulcers.
Mild Symptoms
-
- Patient education on avoiding trauma (e.g. hard foods).
- First-line pharmacological treatment should be topical, and if ineffective, then systemic.
- Pain management:
- Topical analgesics:
- 15% Benzydamine HCl oral rinse applied 4x daily for 2 weeks or until ulcer healed.
- 5% Lidocaine gel applied 4x daily for 2 weeks or until ulcer healed.
- Inflammation control:
- Topical corticosteroids:
- 1% Triamcinolone acetonide dental paste applied 4x daily for 2 weeks or until ulcer healed.
- 05% Fluocinonide cream applied 4x daily for 2 weeks or until ulcer healed.
- Topical corticosteroids:
- Frequency/Duration reduction:
- Antimicrobial mouthwashes:
- 12% Chlorhexidine gluconate mouthwash used 4x daily for 2 weeks or longer.
- Antimicrobial mouthwashes:
- Topical analgesics:
Severe Symptoms
-
- Topical therapies (above) in combination with systemic corticosteroid treatment are recommended.
- 30 – 60 mg Oral prednisone for 1 week, followed by 1-week taper.
- Consider referral to a dental specialist.
- Topical therapies (above) in combination with systemic corticosteroid treatment are recommended.
-
A 2012 Cochrane review of systemic therapies for aphthous stomatitis found no single effective treatment due to lack of drug trials or poor methodology for those that exist.
Quality Of Evidence?

High
We are highly confident that the true effect lies close to that of the estimate of the effect. There is a wide range of studies included in the analyses with no major limitations, there is little variation between studies, and the summary estimate has a narrow confidence interval.
Moderate
We consider that the true effect is likely to be close to the estimate of the effect, but there is a possibility that it is substantially different. There are only a few studies and some have limitations but not major flaws, there are some variations between studies, or the confidence interval of the summary estimate is wide.
Low
When the true effect may be substantially different from the estimate of the effect. The studies have major flaws, there is important variations between studies, of the confidence interval of the summary estimate is very wide.
Justification
- Treatment of RAS with topical corticosteroids has moderate quality evidence. There are a limited number of studies that found statistically significant results compared with placebo.
- Treatment of RAS with systemic corticosteroids has moderate quality evidence. There are a limited number of studies that found statistically significant results compared with placebo. However, they also have high or unclear risk of bias.
Related Information
Reference List
Recurrent aphthous stomatitis.
Akintoye SO, Greenberg MS. . 2014 Apr;58(2):281-297.
Dent Clin North AmAphthous Stomatitis. [Updated 2020 Aug 8]
Plewa MC, Chatterjee K. . In: StatPearls [Internet].
Treasure Island (FL): StatPearls Publishing; 2020 Jan.Aphthous Ulceration.
Scully C. N Engl J Med. 2006;355(2):165-172.Systemic interventions for recurrent aphthous stomatitis (mouth ulcers). Cochrane Database of Systematic Reviews 2012, Issue 9.
Brocklehurst P, Tickle M, Glenny A-M, Lewis MA, Pemberton MN, Taylor J, Walsh T, Riley P, Yates JM. Art. No.: CD005411.Treatment of recurrent aphthous stomatitis. A literature review.
Belenguer-Guallar I, Jimenez-Soriano Y, Claramunt-Lozano A.J Clin Exp Dent. 2014 Apr;6(2):168-174.- Guideline for the Diagnosis and Treatment of Recurrent Aphthous Stomatitis for Dental Practitioners. J Int Oral Health.
Tarakji B, Gazal G, Al-Maweri SA, Azzeghaiby SN, Alaizari N. 2015 May;7(5):74-80.
Relevant Resources
RELEVANT RESEARCH IN BC
Sepsis and Soft Tissue InfectionsRESOURCE AUTHOR(S)

DISCLAIMER
The purpose of this document is to provide health care professionals with key facts and recommendations for the diagnosis and treatment of patients in the emergency department. This summary was produced by Emergency Care BC (formerly the BC Emergency Medicine Network) and uses the best available knowledge at the time of publication. However, healthcare professionals should continue to use their own judgment and take into consideration context, resources and other relevant factors. Emergency Care BC is not liable for any damages, claims, liabilities, costs or obligations arising from the use of this document including loss or damages arising from any claims made by a third party. Emergency Care BC also assumes no responsibility or liability for changes made to this document without its consent.
Last Updated Nov 23, 2020
Visit our website at https://emergencycarebc.ca
COMMENTS (0)
Add public comment…


POST COMMENT
We welcome your contribution! If you are a member, log in here. If not, you can still submit a comment but we just need some information.